Traumatic shoulder instability
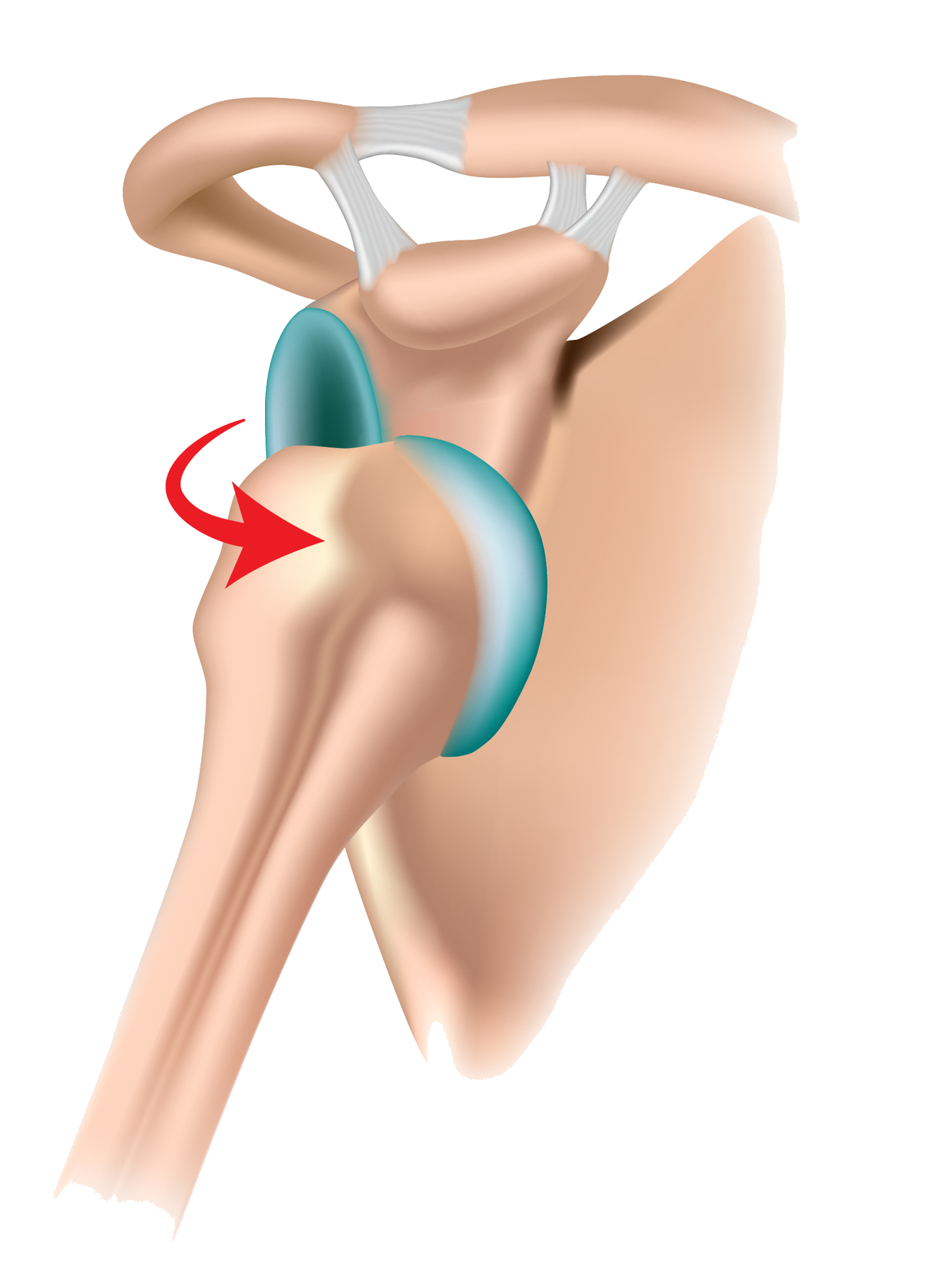
In the shoulder, instability describes when the ball of the humerus moves excessively in the socket. This can be a subluxation which is a partial transient dislocation, or a full dislocation where it comes completely out of the socket. Instability can occur following a specific traumatic event or in some people who naturally have more flexible tissues, who are “double-jointed”. This page refers to those people who have had a specific injury to the shoulder leading to instability.
Instability in the shoulder can be anterior instability where the ball (head) of the humerus has a tendency to come out of the front of the socket (glenoid), or posterior instability, where the heads has a tendency to come out of the back of the glenoid. It generally follows from a specific injury to the shoulder such as a complete dislocation.
The shoulder may initially be painful after a dislocation as some of the soft tissues can be torn and in some cases is associated with a small piece of bone breaking off the socket. While the pain often settles over the following weeks, you may be left with a shoulder that you do not trust, or one that is uncomfortable in certain positions. Some people experience ongoing pain and a catching or clicking in the shoulder. If you have torn some of the muscles around the shoulder when you dislocated it, then you may also notice some weakness.
The best treatment will depend on a large number of factors, both relating to the individual (age, favoured activities, previous injuries to the shoulder, general flexibility) and the injury (which parts of the shoulder were injured).
Physiotherapy is often enough to stabilise the shoulder, working particularly well in older patients. Unfortunately the younger you are when you dislocate your shoulder, the more likely it is to dislocate again and the less likely physiotherapy alone will be sufficient.
Depending on a variety of factors it may be that the surgery can be performed through several small cuts around the shoulder (keyhole surgery), or it may require an open (cut on the front of the shoulder) approach. The torn labrum with or without a small piece of bone may need to be repaired back to the glenoid. Sometimes the divet in the humeral head creates instability and may need to be filled with capsule and tendon tissue (remplissage). Sometimes the shoulder capsule needs to be tightened (shifted), or a more structural procedure performed. This latter procedure may involve moving a piece of bone to the front of the shoulder from the hip (iliac crest) or elsewhere in the shoulder region (coracoid process) and is known as a Latarjet procedure.
Following surgery you will be in a sling. You can come out of the sling for physiotherapy. From 3 weeks after your surgery you will start to come out of the sling during the day but continue to wear it at night. At 6 weeks you will have discarded the sling and you will work on any residual stiffness in the shoulder before progressing to strengthening work at around 12 weeks from surgery. Light 2 handed activities can commence at 3-6 weeks and moderate lifting at 3 months.
Following surgery the shoulder usually feels more secure and the aim is that you are able to use it and trust it not to dislocate. It can still dislocate if enough force is applied, similar to how it first dislocated, so it does not make the shoulder indestructible. The shoulder will also be a bit stiffer, especially initially following the surgery but this often stretches out with time.